03/30/2022
Introduction
Back pain between the shoulder blades, or what the medical field might call the interscapular region, means pain in the back of our upper trunk, or the thoracic region of the spine. While pain in the neck or low back is much more common, pain in the thoracic region may affect up to 30 percent of people in their lifetime. In order to understand where this interscapular pain may be coming from, let’s start with some anatomy.
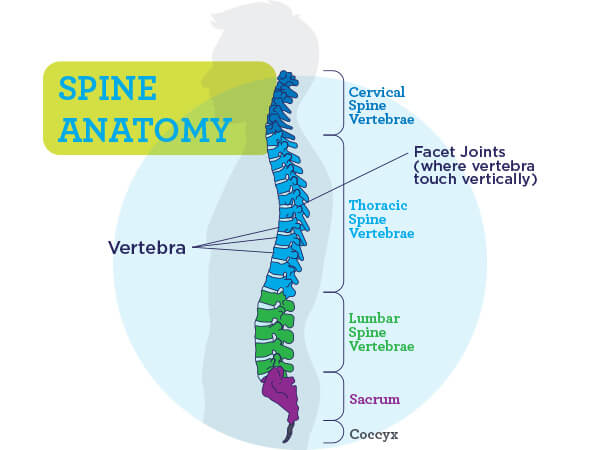
Our spines, from top to bottom, consist of (see Spine Anatomy image):
Cervical portion (7 vertebrae): supports the weight of our heads
Thoracic portion (12 vertebrae): attaches to our ribs to protect our heart and lungs
Lumbar portion (5 vertebrae): supports the weight of our bodies
Tailbone, the sacral vertebrae (5 fused vertebrae): provides a connection to our hips
Between each of the non-fused vertebra there is a disc, or a soft spongy shock absorber, to provide some cushion between the rigid bones and to allow the spine to move in different directions.
The spinal cord connects the brain to the body and travels through a bony canal toward the back portion of the spine, created by stacking one vertebrae on top of the next one down. The bone at the front of the vertebrae, the vertebral body, provides the strength and support for our heads and bodies, and the bone on the back of the vertebra creates a bony ring to protect the spinal cord. Stacking one vertebra and its bony ring on top of the next creates the spinal canal for the spinal cord to travel from our head toward our tailbone.
The nerves that go out to our bodies arise from the spinal cord. A spinal nerve exits at each level between any two vertebrae in the cervical, thoracic, lumbar, and sacral spine. The spinal nerves are mixed nerves, with components for the muscles (motor), our skin (sensory), and our organs (autonomic). Pain describes an uncomfortable sensation in our bodies, and this sensation is transmitted from our bodies to the spinal cord through these nerves, and then through the spinal cord to the brain.
Pain can be categorized in many ways, but a good starting point is to think of acute pain and chronic pain. Acute pain comes on suddenly, is frequently caused by damage to our soft tissues, bones, or organs, and is expected to resolve. Examples might be pain related to a muscle strain or ligament sprain, trauma, or a spontaneous event involving one of our organs, such as a perforated ulcer. Chronic pain is typically present for more than 3-6 months and is usually associated with a long-term or chronic illness. This may be a degenerative process like osteoarthritis, an inflammatory process like rheumatoid arthritis, or direct injury to the nerves themselves.
As we focus on the interscapular region, the area between our shoulder blades, we can think of it in layers. Later, this will help us determine where the pain is coming from and our best treatment plan. From the outside in, we first have the skin, then the next layer down we have the soft tissues and muscles, then the spine with its bones, discs, joints between the vertebrae themselves and the joints between the vertebrae and the ribs, and finally the heart and lungs in the chest cavity in front of the spine. We could have an acute injury to any of the tissues in these layers that would cause acute pain, or there could be a long-term or chronic illness that could affect these tissues, too, and cause chronic pain.
Causes of Back Pain Between the Shoulder Blades
Let’s start with some of the causes for pain between the shoulder blades, looking at the layers from the outside in.
- 01
Skin
Acute injuries to the skin in this region usually have an obvious explanation, such as a burn or chemical irritation. These injuries are treated symptomatically, and the pain should resolve.
There are examples of chronic pain that involve the skin in the interscapular region that may require ongoing symptom and pain management. Although relatively uncommon, they may cause distress when present.
One example is shingles, a common condition developed later in life by people who had Chicken Pox when they were younger. Usually, the pain resolves as the shingles rash subsides, but in about 10 percent of people with shingles, there may be chronic burning pain, known as post-herpetic neuralgia. Another example of a chronic sensory complaint that involves the skin in the area between the shoulder blades is notalgia paresthetica, a dermatologic complaint with one-sided itching between the spine and the shoulder blade. Again, this dermatomal distribution indicates involvement of the upper thoracic spinal nerves. This condition may have also prompted the invention of the “back scratcher” for this hard-to-reach location.
- 02
Soft Tissues and Muscles
The next layer includes the soft tissues immediately beneath the skin and the muscles. The two main muscle groups in the interscapular region are the trapezius muscle and the rhomboid muscles (major and minor). The trapezius muscle starts at the base of the neck, spreads across the shoulders, and extends to the middle of the back. Between the shoulder blades the trapezius muscle pulls the shoulders back, brings the shoulders down, and stabilizes the spine with twisting and bending. The rhomboid muscles are immediately deep to the trapezius, arise from the tips of the upper thoracic vertebrae, and attach to the inside edge of the shoulder blade. These muscles stabilize the shoulder blade and shoulder with arm and upper body movement, important in pulling, throwing, and overhead arm movement.
One of the most common causes of pain between the shoulder blades is a muscle strain of the trapezius or rhomboid muscles, in which the muscle fibers are stretched or torn. This may occur with exercises, lifting, or carrying, or any other activities that require pulling, throwing, overhead arm movement or pulling the shoulders down. Typically this will cause acute pain that is initially managed with rest, ice, and anti-inflammatory medications. Direct force or blunt trauma to this region, such as with a fall or a motor vehicle accident, may also cause bruising and inflammation of the muscles and surrounding tissues and cause acute pain. Poor posture may cause prolonged stress on these muscles that also causes pain.
Another cause of pain between the shoulder blades is myofascial pain, pain arising from the muscles (myo-) and the coverings of the muscles, or fascia (-fascial). Whereas muscle strain, trauma, and poor posture may cause acute pain between the shoulder blades, myofascial pain that lasts more than 6 months represents a chronic form. The pain is usually localized, and there may be trigger points on the involved muscles. Vitamin D deficiency may contribute to myofascial pain. Dry needling by a physical therapist, injection of local anesthetic into trigger points, acupuncture, and Vitamin D supplement have demonstrated therapeutic effects.
- 03
Spine
The deepest layer in the interscapular region includes the spine, with the vertebrae, discs, and ribs attached to the vertebrae. Injuries to the vertebrae, the discs between the vertebrae, or the joints between the ribs and the vertebrae may all cause pain between the shoulder blades.
Fractures of the vertebrae in the upper thoracic spine will cause interscapular pain. Fractures secondary to trauma, such as a fall or motor vehicle accident, may be treated with bracing or surgical stabilization, depending on the type of fracture. Fractures may also result from bone weakening due to osteoporosis or tumor involvement in the bone. Compression fractures related to osteoporosis more likely occur in the lower thoracic spine, but may occur in the upper thoracic spine and cause pain between the shoulder blades. These fractures are typically treated with an external brace or with vertebroplasty or kyphoplasty, a procedure in which a cement mixture is injected into the vertebra for internal stabilization.
Thoracic disc degeneration and thoracic disc herniation are common, but do not necessarily cause pain. In a study of 90 asymptomatic patients using magnetic resonance imaging (MRI), over 70% had thoracic disc degeneration and over 35% had thoracic disc herniations. Usually these MRI findings are not the cause of pain between the shoulder blades, however. Thoracic disc herniations that are symptomatic either cause spinal cord compression, that typically does not cause pain but does cause loss of spinal cord function, or cause thoracic spinal nerve root compression, that causes pain that radiates to the mid back and chest wall, the nerve’s dermatome.
Infections in the upper thoracic vertebrae (osteomyelitis) or the discs ( discitis) may cause pain between the shoulder blades. These infections are usually treated with antibiotics, although surgery may be required in some situations.
Tumors that involve the upper thoracic vertebrae may cause pain, even without fracture. These tumors are usually managed by a cancer doctor, also known as an oncologist. Treatment may include chemotherapy or radiation therapy. Surgical treatment is indicated in select cases.
Severe scoliosis, or sideways curvature of the spine, may cause stress on the spine and joints that causes pain. Treatment recommendations may include physical therapy, bracing, or surgical correction.
Inflammatory conditions such as rheumatoid arthritis may involve the joints in the spine and cause pain. These conditions are typically managed with medications, usually under the direction of a rheumatologist.
- 04
Chest Cavity and Organs
The thoracic vertebrae in our trunk region attach to the ribs and create the chest cavity that protects our heart and lungs. The esophagus connects the mouth to the stomach and also passes through the chest cavity. Because the chest cavity is immediately in front of the interscapular region, illnesses or diseases that involve any of the organs in the chest cavity may also cause pain between the shoulder blades. The pain may be either acute or chronic, depending on the cause and the organ involved.
Let’s consider some examples:
Heart: a heart attack (myocardial infarction) may cause pain between the shoulder blades as well as in the chest. Pain between the shoulder blades from a heart attack occurs more commonly in women than men. Obviously, this is a medical emergency.
Blood vessels: someone with a thoracic aortic aneurysm may experience leaking or rupture of the aneurysm, which may cause pain between the shoulder blades. This is also a medical emergency.
Lungs: a pulmonary embolus (PE) can block blood flow to a portion of the lung, causing lung tissue to be damaged and sometimes, depending on the location of the lung tissue involved, this may also cause interscapular pain. This too is a medical emergency. Another cause for pain between the shoulder blades may be related to a lung tumor, again, depending on its precise location.
Gastrointestinal: acid reflux, or gastroesophageal reflux disease (GERD), describes the movement of acidic stomach contents from the stomach upward into the esophagus. The acidic fluid irritates the tissues of the esophagus and may cause interscapular pain. Gallbladder disease may also cause pain between the shoulder blades. This is what’s known as referred pain.
Referred pain: in addition to referred pain from gall bladder disease that is located between the shoulder blades, an inflamed or pinched nerve in the neck may cause interscapular pain (between the shoulder blades). Patients with a symptomatic disc herniation in the neck, pinching a cervical nerve root, characteristically have pain that radiates from the neck to the area between the spine and the shoulder blade on the affected side, in addition to pain in the shoulder and arm on that side.
Evaluation of Back Pain Between the Shoulder Blades
- 01
History
The first step in the evaluation of pain between the shoulder blades is understanding the history and characteristics of the pain. Your health care provider needs to ask a series of questions to understand the location of the pain, how rapidly it came on, the type of pain, things that make it worse or better and associated symptoms. These questions may include:
- Where is your pain located?
- Is it on one side or both?
- How long have you had this pain?
- Did it come on suddenly or gradually?
- Were you doing any particular activity when it started?
- Have you ever had pain like this before?
- How severe is the pain?
- What does the pain feel like – for example, is it aching, sharp, stabbing, throbbing, burning?
- Is there anything that makes the pain better or worse?
- Are there any associated symptoms, like numbness or tingling in the arms, chest pain, shortness of breath, weight loss, fever?
The answers to these questions (and follow-up questions) may provide some very important clues regarding the cause of the pain.
- 02
Physical Examination
The next step in the evaluation is to perform a physical examination. Your health care provider will want to examine the area between the shoulder blades to assess for skin changes, palpate (touch) the soft tissues in this region for tenderness and the location of the pain, and assess the surrounding structures such as the spine and shoulder blade to help determine if those structures are involved.
- 03
Imaging
Depending on the results of the history and physical examination, imaging studies may be necessary to further evaluate the pain. Plain x-rays may be taken of the cervical or thoracic spine, the chest, or the shoulder, a CT study may be performed for the spine or the chest, and an MRI study may be needed for the cervical or thoracic spine or the shoulder. Each of these studies allows us to see the aforementioned layers in different ways, so it’s possible multiple studies may be conducted.
Diagnosis and Treatment of Back Pain Between the Shoulder Blades
The diagnosis for the source of the pain will be reached after completing the history and physical examination, and reviewing any imaging studies that were obtained.
The recommended treatment is entirely dependent on the diagnosis of the cause of the pain between the shoulder blades.
Lesions of the skin may require symptomatic treatment or medications, only. A dermatologist may be referred to as they are the best person to recommend appropriate treatment for these problems.
A strain of the trapezius or rhomboid muscles, the most common cause of pain between the shoulder blades, may be treated with rest, ice, and non-steroidal anti-inflammatory medications. A more severe strain may lead to enrollment in physical therapy. Chronic pain between the shoulder blades may also be managed by a pain management specialist, especially if injection procedures are recommended.
Fractures of the spine may be treated with bracing or surgical stabilization. Inflammatory conditions of the spine such as back arthritis or a herniated disc often require medical or surgical management, depending on the severity of the condition and its impact on your day-to-day activities.
Pain arising from organs in the chest cavity will require a specific treatment plan depending on the organ involved. These conditions may be medical emergencies and typically would result in a referral to a non-orthopaedic specialist.
Conclusion
Pain between the shoulder blades is a common condition that affects up to 30 percent of people in their lifetime. Most often this is related to a strain of the muscles between the spine and the shoulder blade and may be precipitated by activities, exercise, or sports. Throwing, reaching, and pulling are movements that may strain these muscles. Treatment for muscle strains in this region includes rest, ice, and non-steroidal anti-inflammatory medications. Patients with more severe strains may benefit from enrollment in physical therapy.
In addition to muscle strains, pain between the shoulder blades may arise from any of the tissues and structures in this region, including the skin, the spine, the ribs, and the organs in the chest cavity. A musculoskeletal specialist can initiate the evaluation for the source of the pain. After a diagnosis is made, a treatment plan will be developed. This may include medications, physical therapy, spine pain injections, surgery, or referral to the appropriate specialist.
As you can see, there is a lot to consider when it comes to back pain between the shoulder blades. A physician who knows the spine well and knows what questions to ask about back surgery – and the follow-up questions to those questions – will be best positioned to make an accurate diagnosis and appropriate treatment plan.
Call (402) 609-3000, text (402) 609-3000 to make an appointment with a spine specialist at OrthoNebraska.